Epidural Steroid Injections
Chronic axial pain is estimated to cost the United States $100 billion per year with approximately 40 million sufferers. This estimate does not include chronic pain caused by malignancy.1 Low back pain specifically is estimated to have the highest burden on the American healthcare system with neck pain coming in at number four.2 In some estimates the prevalence of low back and neck pain within an individual’s lifetime is as high has 80%. Epidural steroid injections are a commonly used form of interventional pain management.
Pain in the low back can be attributed to many causes and tissue types. These causes include, spinal facet injury, muscle spasm, degeneration of the disc, herniation of the disc, spinal stenosis and referral from other sources such as the sacroiliac joint. Often an individual can have multiple causes at once. Common complaints include: stiffness, dull sensations, sharp sensations and radiation of pain often into the leg.
Discogenic pain, meaning pain originating from the intervertebral disc, is a common injury that can be felt at the source of pain as well as referred pain into the hip region, groin and radiating pain into the leg. This is often accompanied by muscle spasm for a brief period. Often referred to as a disc herniation, bulge or protrusion, disc injury can be incredibly painful, impacting even basic daily activities. Similar symptoms can be seen in the neck.

In cases where an individual’s pain is discogenic (caused by any injury to the intervertebral disc) or caused by an inflammatory response affecting the nerve root, the utilization of an epidural steroid injection (ESI) may be indicated. Epidural steroid inject is a procedure utilized to decrease inflammation an
d irritation within the spine. In an orthopedic setting an ESI is can help with chronic low back, mid-back or neck pain. Among a variety of non-surgical procedures intended to treat axial pain, ESI is one of the most common.
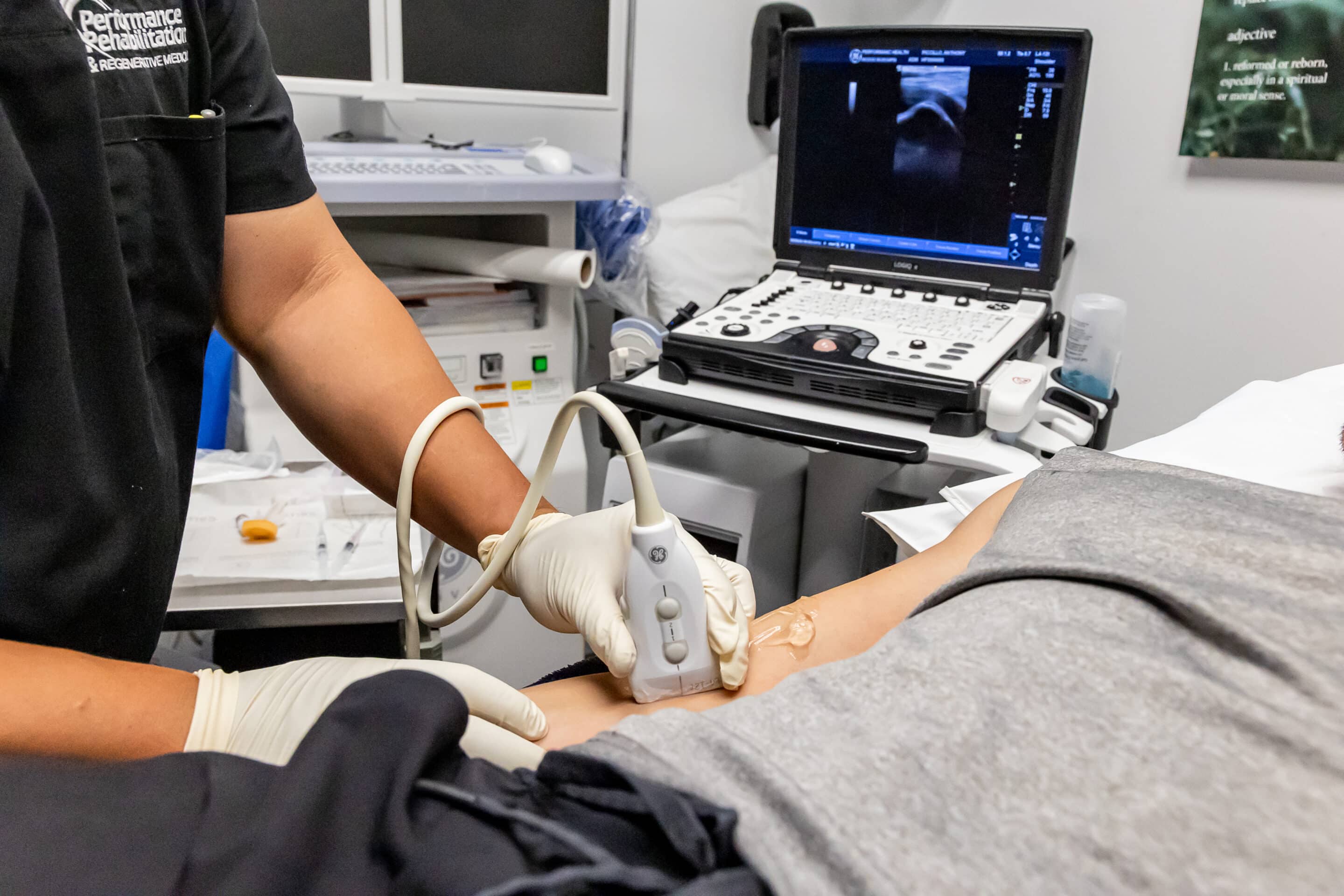
Image-Guided Epidural Steroid Injection
The procedure is image-guided, injection based containing a local anesthetic and corticosteroid. The anesthetic is used for short-term pain relief while the corticosteroid is meant to provide long-term relief. The solution is injected into the epidural space of the spinal cord, which is the outermost section of the spinal cord and contains the spinal nerve root.
An ESI can be administered in three types: caudal, interlaminar and transforaminal. The interlaminar approach is from the posterior and is administered between the lamina of the spinal segment above and below. It is reported to be the most common as it is can deliver the medication closest to the injury site. Transforaminal application is a more lateral approach that focuses on the space when the nerve root exits. It has shown to use the least medication due to its specificity at an individual segment. Caudal approach is from the inferior portion and is used exclusively in the lumbar spine. It is considered to be the easiest of the three procedures but is the least specific and requires the most medication.3 In many cases an individual patient may receive multiple approaches based on their reaction to other procedures, ongoing symptoms and diagnostics performed.
A recent systematic review of the use of ESI for chronic spinal pain examined its use with the objective of assessing the treatments efficacy on chronic low back pain of a discogenic or stenotic nature.4 The study reviewed 630 per review studies, grading each prior study and categorizing them into five levels with level I being of the highest quality. It contained randomized controlled trials, observational studies and opinion or consensus of groups of clinicians or scientists. Level I grade is considered to be evidence obtained from multiple high quality randomized trials. Level II is evidence obtained from one high level or multiple moderate or low level randomized trials. Correlating evidence from
To summarize the findings, there is a high level of evidence supporting the use of ESI in the cervical and lumbar spine in the management of axial pain. Although it has not been discussed in this essay, the review by Kaye et al also showed a moderate level of evidence to support the use of ESI in the thoracic spine.
In many cases, a cost analysis is important in examining the use of one procedure over another. In the case of the epidural steroid injection, it is shown to be more cost affective when compared to spinal cord stimulator or surgical intervention.5 Other outcomes in determining success have been examined including magnetic resonance imaging and epidural contrast flow pattern but have not shown significant results thus far.6
Although some complications have been seen, specifically in the use of transforaminal approach in the cervical spine, the use of ESI throughout the spinal column to treat discogenic and stonic type conditions has strong evidence to support its use. In a clinical setting it is strongly suggested that the clinician take all factors into account before any type of procedure. Continued studies are encouraged to further the understanding of the treatment and its implications. Practitioners that are considering ESIs are advised to seek out the most recent literature to guide in their clinical decision-making
About the Authors
Joseph Mejia D.O., F.A.A.P.M.& R, is a graduate of University of Michigan and West Virginia School of Osteopathic Medicine. He is Board Certified in Physical Medicine & Rehabilitation and Sports Medicine. Dr. Mejia received his Fellowship Training in Interventional Pain Management from University of Medicine and Dentistry. He has advanced training in Regenerative Medicine and is the Medical Director and Partner of Performance Rehabilitation & Regenerative Medicine.
John F. Ellis, D.C. is a graduate of Logan Chiropractic College. He is a Board Certified Chiropractic Physician with licenses held in New Jersey and New Hampshire. His past research work involves human performance pertaining to orthopedic conditions. Dr. Ellis is a Chiropractic Physician at Performance Rehabilitation & Regenerative Medicine.
References:
- Gaskin DJ, Richard P. The economic costs of pain in the United States. J Pain 2012; 13:715-724.
- US Burden of Disease Collaborators. The state of US health, 1999-2010: Burden of diseases, injuries, and risk factors. JAMA 2013; 310:591-608.
- Manchikanti L et al. An update of comprehensive evidence-based guidelines for interventional techniques of chronic spinal pain: Part II: Guidance and recommendations. Pain Physician 2013; 16:S49-S283.
- Kaye D et al. Efficacy of Epidural Injection in Managing Chronic Spinal Pain: A Best Evidence Synthesis. Pain Physician 2015; 18:E939-E1004
- Manchikanti L, Falco FJE, Pampati V, Cash KA, Benyamin RM, Hirsch JA. Cost utility analysis of caudal epidural injections in the treatment of lumbar disc herniation, axial or discogenic low back pain, central spinal stenosis, and post lumbar surgery syndrome. Pain Physician 2013; 16:E129-E143.
- Mallinson PI, Tapping CR, Bartlett R, Maliakal P. Factors that affect the efficacy of fluoroscopically guided selec- tive spinal nerve root block in the treatment of radicular pain: A prospective cohort study . Can Assoc Radiol J 2013; 64:370-375.